O&P Design Software: Why Clinical Control Matters More Than Automation
Explore how modern O&P design software is evolving beyond presets to give clinicians full control over prosthetic socket design, improving accuracy, consistency, and patient outcomes.
BENX PLATFORM
4/24/202610 min read
O&P Design Software should support Clinical Thinking, not replace it
Introduction
In orthotics and prosthetics, outcomes depend on one thing above all else: clinical judgment. No two limbs are the same. No two patients respond the same way to pressure, alignment, or support. Yet, many digital tools in the market still rely heavily on presets and automated assumptions.
At first glance, that feels efficient. But in practice, it often creates a gap between what the clinician intends and what the software produces. That gap leads to rework. Adjustments. Compromises.
The future of prosthetic socket design is not about removing clinicians from the process. It is about giving them better tools to apply their expertise with greater precision, consistency, and efficiency. The best O&P software does not replace clinical judgment, it amplifies it.
The problem begins before design even starts
Most assume socket design issues begin during modeling. In reality, they start at the scan.
In real clinical environments, scan data is rarely perfect. You deal with:
Noise and surface irregularities
Missing regions
Soft tissue distortion
Scanner limitations
As a result, significant time is spent cleaning and correcting data before actual design even begins.
A more effective approach is to prepare scan data intelligently before it reaches the design stage. This includes:
Mesh repair to fix structural gaps
Surface smoothing without losing anatomy
Orientation and scale normalization
Stabilizing soft tissue artifacts
When inputs are clean and reliable, everything that follows becomes easier. Better inputs lead to fewer corrections and more predictable outcomes.
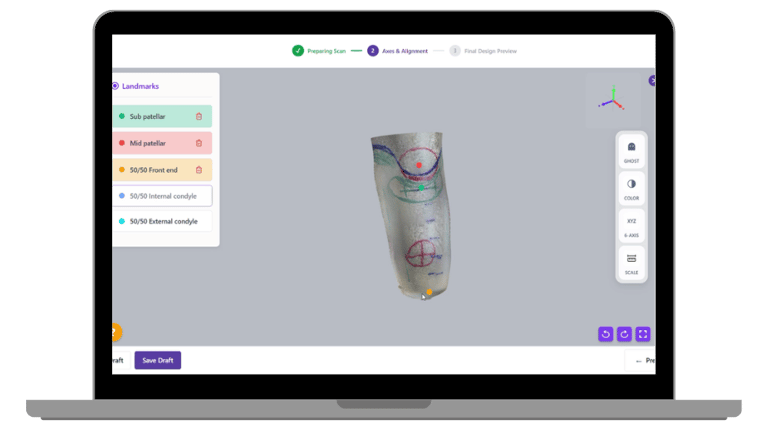
Alignment should be seen, not assumed
Small alignment errors at the digital design stage can affect load distribution, comfort, gait, and overall socket performance. Yet many workflows still rely on manual approximation and repeated adjustments.
It is still approximated in many workflows. You tweak and verify and tweak. It’s an iterative process. A better system does not add more tools. It enhances clarity.
When clinicians can see orientation in real time, they are able to:
Immediately understand positioning of limbs
Move faster
Design with greater confidence
That change alone cuts uncertainty. Less uncertainty leads to greater consistency.
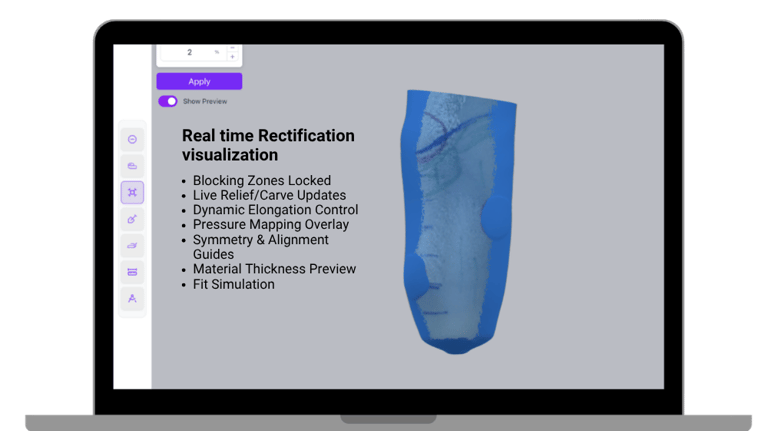
Rectification is where clinical expertise matters most
This is the stage where a clinician’s experience translates into geometry. But digital tools often struggle here. Feedback may be delayed, transitions can feel unnatural, and control often feels limited. As a result, the final model may not fully reflect clinical intent.
A more refined approach focuses on making rectification behave closer to hands-on practice.
Changes respond instantly
Adjustments stay localized
Transitions remain smooth and anatomical
This allows the design to evolve in a way that feels natural, not forced. When digital rectification mirrors the way clinicians think and work, expertise translates more accurately into the final socket geometry. The result is greater consistency without sacrificing personalization.
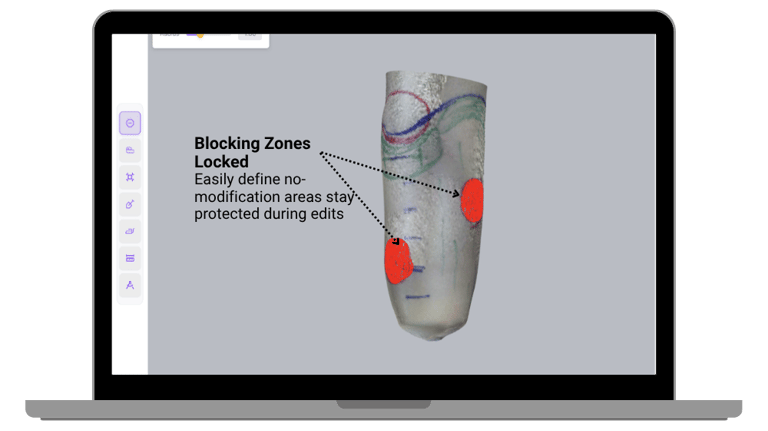
Blocking should feel controlled, not corrective
Blocking defines relief and load-bearing zones. But in many workflows, it quickly becomes inconsistent and difficult to control. Edges may be irregular. Adjustments feel unpredictable. Corrections pile up downstream. This creates unnecessary complexity.
When blocking is precise and controlled from the start:
Regions are clearly defined
Transitions are smooth
Depth adjustments are predictable
The result is a cleaner design that requires fewer fixes later.
Geometry should follow anatomy, not distort it
One of the subtle but important challenges in digital design is maintaining natural contours.
During carving or reduction, it’s easy to create:
Sharp dents
Artificial edges
Loss of anatomical continuity
A better system ensures modifications respect natural limb geometry. Smooth anatomical carving allows reductions without compromising shape integrity.
This is where digital tools need to feel less mechanical and more intuitive.
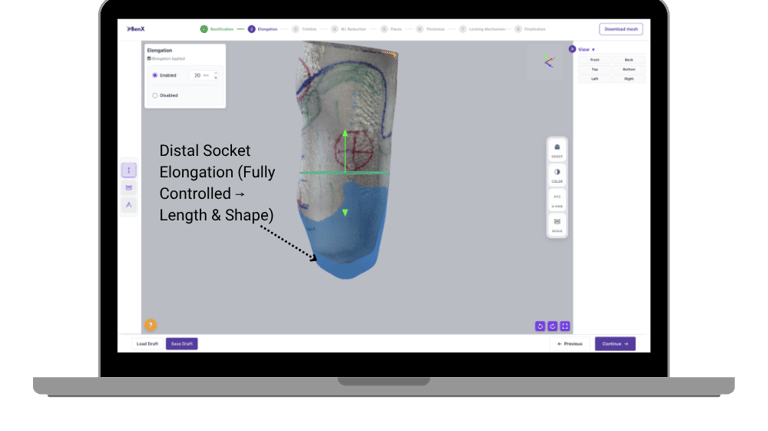
Elongation should not be trial and error
Socket elongation often becomes an iterative process of repeated adjustments. Too much extension affects comfort. Too little requires rework. This back-and-forth slows down the process.
A more controlled approach uses geometry-aware behavior:
Extensions follow natural contours
Trimlines develop predictably
Adjustments feel guided, not random
This reduces iteration and improves efficiency.
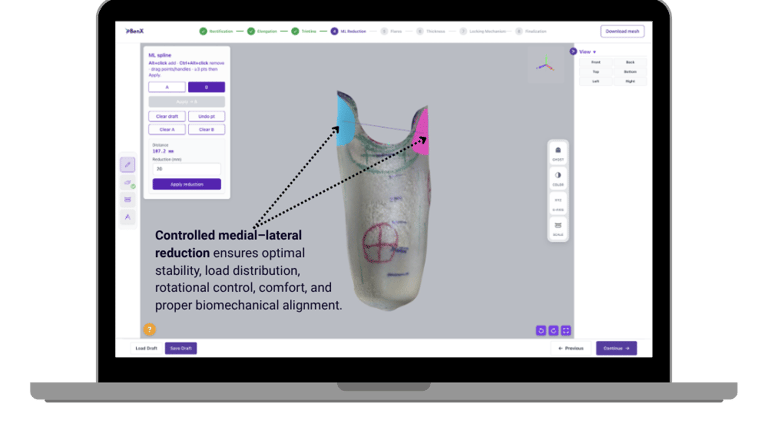
Reduction should be consistent across cases
Reduction is one of the most experience-driven steps. But even experienced clinicians can see variation due to time pressure or workflow differences.
Digital tools can help here - not by replacing judgment, but by supporting it.
Intelligent reduction tools can provide:
Geometry-aware recommendations
Region-specific reduction controls
Consistent starting points for clinicians
Full flexibility to modify or override suggestions
This maintains clinical authority while improving repeatability. Consistency improves outcomes. And consistency is what scales.
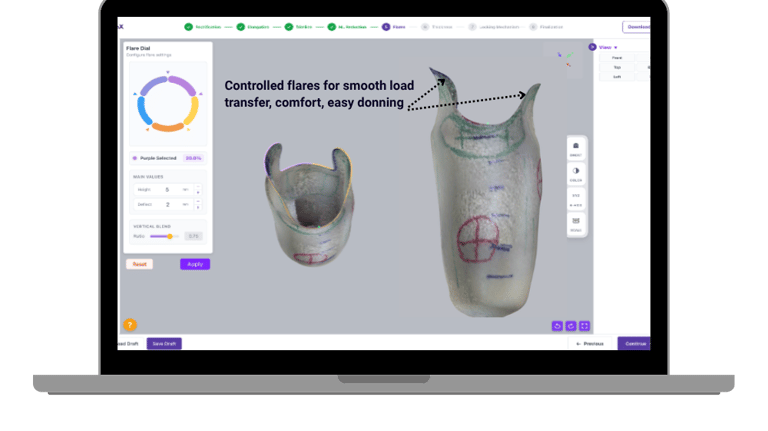
Flare design impacts comfort more than expected
Flare is often treated as a minor finishing step. But in reality, it directly affects how the socket feels during use.
Poor flare design can lead to:
Sharp edges
Uneven transitions
Additional trimming during fitting
When flare is designed intentionally from the beginning:
Edges feel smoother
Transitions are controlled
Fitting adjustments reduce
Small improvements here make a big difference in patient comfort.
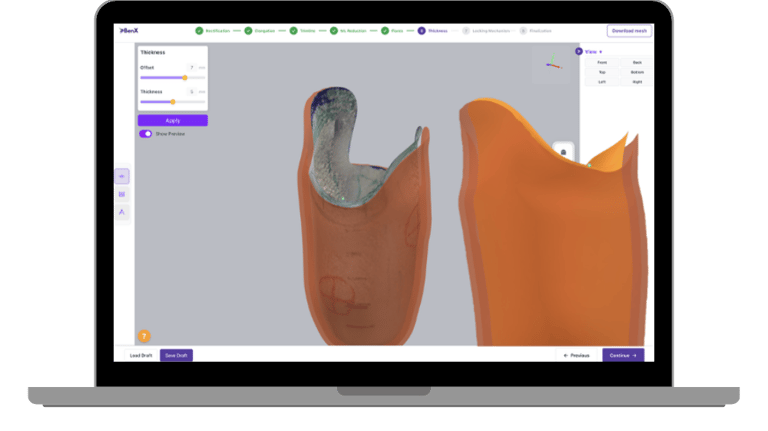
Thickness should reflect real biomechanics
Sockets do not experience uniform load. Some regions need strength. Others benefit from flexibility. Uniform thickness fails to reflect this reality.
A more advanced approach allows:
Region-based thickness control
Smooth transitions between zones
Structural integrity during fabrication
This turns thickness into a functional design element rather than a fixed parameter.
Integration should happen early, not later
Components like locking systems are often added at the end. This can lead to alignment issues, structural compromises, and manufacturing challenges.
When integration is considered during design:
Components align naturally
Load paths remain consistent
Reinforcement is built in
Fabrication requirements are considered early
A socket design is only successful if it can be manufactured accurately and consistently. When design and manufacturing considerations work together from the beginning, clinics achieve greater repeatability, fewer remakes, and more predictable patient outcomes.
What you design should match what you manufacture
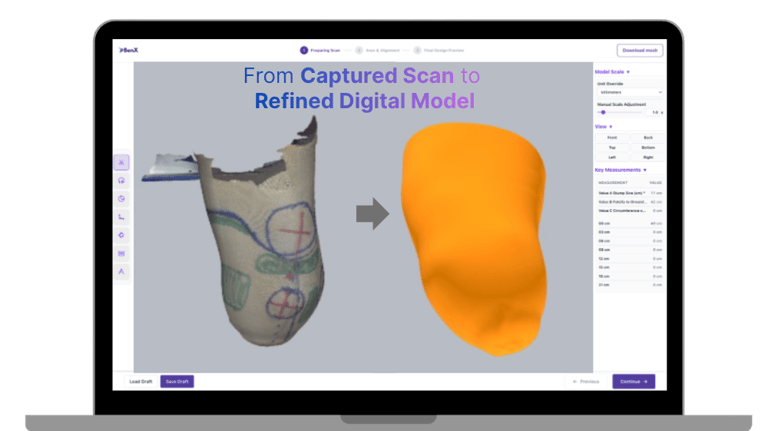






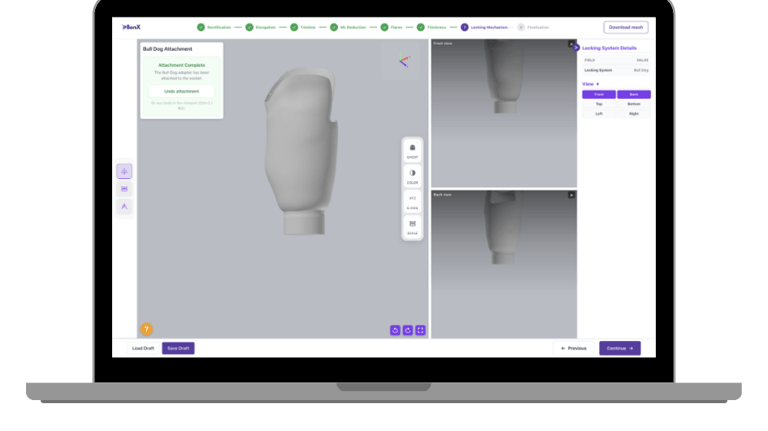
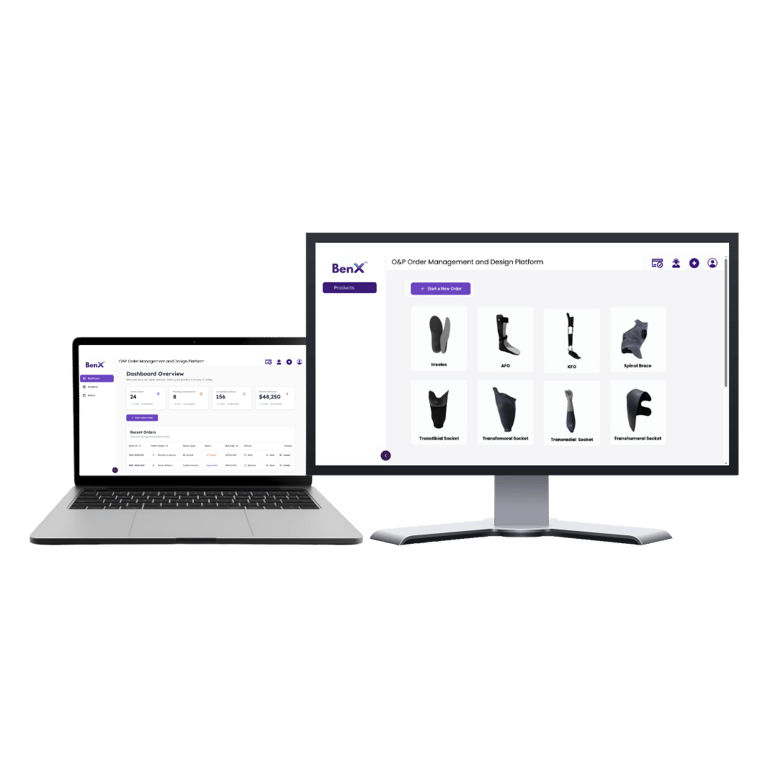
A clean digital model does not always translate into a clean physical socket. Surface artifacts, mesh issues, or inconsistencies can affect fabrication. That is why fabrication readiness should not be treated as a final step.
It should be maintained throughout the workflow.
Clean mesh structure
Smooth surface continuity
Stable export geometry
When design and manufacturing align, outcomes improve significantly.
Final thoughts
From Iteration to Intention
Technology should not dilute clinical expertise. It should amplify it.
Traditional socket design is iterative: Adjust→Test→Correct→Repeat. But it does not have to stay that way.
With the right O&P design software, the goal shifts from iteration to intention. Each step becomes clearer. Each decision more controlled.
Not by adding complexity, but by improving Clarity, Consistency and Clinical control.
The future of O&P design software lies in giving clinicians the ability to apply their judgment with greater precision and confidence.
Not through presets.. but through control.
If you are involved in prosthetic or orthotic design and want to explore a more controlled, clinically driven workflow, BenX is currently open for early beta access to a limited group of clinicians.
If this approach aligns with how you think about design, we would be glad to connect.
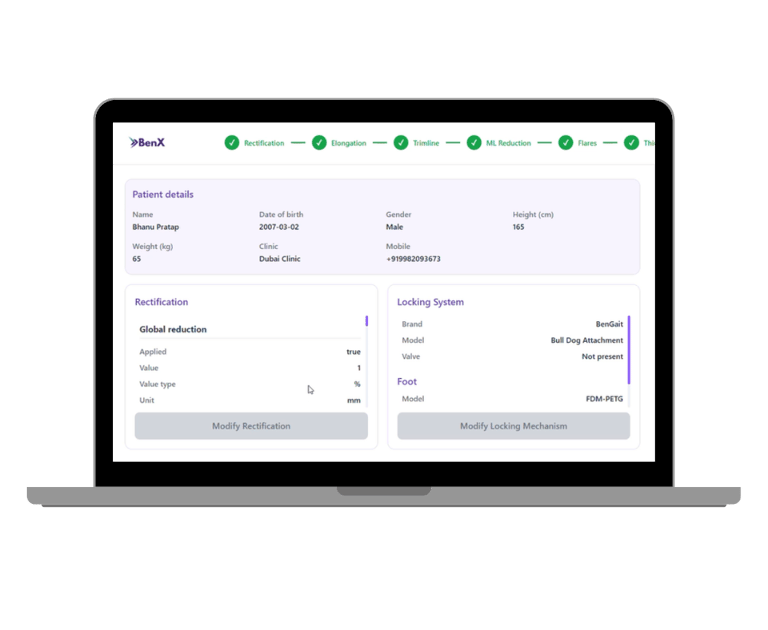
O&P Design Software should support Clinical Thinking, not replace it
Introduction
In orthotics and prosthetics, outcomes depend on one thing above all else: clinical judgment. No two limbs are the same. No two patients respond the same way to pressure, alignment, or support. Yet, many digital tools in the market still rely heavily on presets and automated assumptions.
At first glance, that feels efficient. But in practice, it often creates a gap between what the clinician intends and what the software produces. That gap leads to rework. Adjustments. Compromises.
The future of prosthetic socket design is not about removing clinicians from the process. It is about giving them better tools to apply their expertise with greater precision, consistency, and efficiency. The best O&P software does not replace clinical judgment, it amplifies it.
The problem begins before design even starts
Most assume socket design issues begin during modeling. In reality, they start at the scan.
In real clinical environments, scan data is rarely perfect. You deal with:
Noise and surface irregularities
Missing regions
Soft tissue distortion
Scanner limitations
As a result, significant time is spent cleaning and correcting data before actual design even begins.
A more effective approach is to prepare scan data intelligently before it reaches the design stage. This includes:
Mesh repair to fix structural gaps
Surface smoothing without losing anatomy
Orientation and scale normalization
Stabilizing soft tissue artifacts
When inputs are clean and reliable, everything that follows becomes easier. Better inputs lead to fewer corrections and more predictable outcomes.
Alignment should be seen, not assumed
Small alignment errors at the digital design stage can affect load distribution, comfort, gait, and overall socket performance. Yet many workflows still rely on manual approximation and repeated adjustments.
It is still approximated in many workflows. You tweak and verify and tweak. It’s an iterative process. A better system does not add more tools. It enhances clarity.
When clinicians can see orientation in real time, they are able to:
Immediately understand positioning of limbs
Move faster
Design with greater confidence
That change alone cuts uncertainty. Less uncertainty leads to greater consistency.
Rectification is where clinical expertise matters most
This is the stage where a clinician’s experience translates into geometry. But digital tools often struggle here. Feedback may be delayed, transitions can feel unnatural, and control often feels limited. As a result, the final model may not fully reflect clinical intent.
A more refined approach focuses on making rectification behave closer to hands-on practice.
Changes respond instantly
Adjustments stay localized
Transitions remain smooth and anatomical
This allows the design to evolve in a way that feels natural, not forced. When digital rectification mirrors the way clinicians think and work, expertise translates more accurately into the final socket geometry. The result is greater consistency without sacrificing personalization.
Blocking should feel controlled, not corrective
Blocking defines relief and load-bearing zones. But in many workflows, it quickly becomes inconsistent and difficult to control. Edges may be irregular. Adjustments feel unpredictable. Corrections pile up downstream. This creates unnecessary complexity.
When blocking is precise and controlled from the start:
Regions are clearly defined
Transitions are smooth
Depth adjustments are predictable
The result is a cleaner design that requires fewer fixes later.
One of the subtle but important challenges in digital design is maintaining natural contours.
During carving or reduction, it’s easy to create:
Sharp dents
Artificial edges
Loss of anatomical continuity
A better system ensures modifications respect natural limb geometry. Smooth anatomical carving allows reductions without compromising shape integrity.
This is where digital tools need to feel less mechanical and more intuitive.
Socket elongation often becomes an iterative process of repeated adjustments. Too much extension affects comfort. Too little requires rework. This back-and-forth slows down the process.
A more controlled approach uses geometry-aware behavior:
Extensions follow natural contours
Trimlines develop predictably
Adjustments feel guided, not random
This reduces iteration and improves efficiency.
Reduction should be consistent across cases
Reduction is one of the most experience-driven steps. But even experienced clinicians can see variation due to time pressure or workflow differences.
Digital tools can help here - not by replacing judgment, but by supporting it.
Intelligent reduction tools can provide:
Geometry-aware recommendations
Region-specific reduction controls
Consistent starting points for clinicians
Full flexibility to modify or override suggestions
This maintains clinical authority while improving repeatability. Consistency improves outcomes. And consistency is what scales.
Flare design impacts comfort more than expected
Flare is often treated as a minor finishing step. But in reality, it directly affects how the socket feels during use.
Poor flare design can lead to:
Sharp edges
Uneven transitions
Additional trimming during fitting
When flare is designed intentionally from the beginning:
Edges feel smoother
Transitions are controlled
Fitting adjustments reduce
Small improvements here make a big difference in patient comfort.
Thickness should reflect real biomechanics
Sockets do not experience uniform load. Some regions need strength. Others benefit from flexibility. Uniform thickness fails to reflect this reality.
A more advanced approach allows:
Region-based thickness control
Smooth transitions between zones
Structural integrity during fabrication
This turns thickness into a functional design element rather than a fixed parameter.
Integration should happen early, not later
Components like locking systems are often added at the end. This can lead to alignment issues, structural compromises, and manufacturing challenges.
When integration is considered during design:
Components align naturally
Load paths remain consistent
Reinforcement is built in
Fabrication requirements are considered early
A socket design is only successful if it can be manufactured accurately and consistently. When design and manufacturing considerations work together from the beginning, clinics achieve greater repeatability, fewer remakes, and more predictable patient outcomes.
What you design should match what you manufacture
A clean digital model does not always translate into a clean physical socket. Surface artifacts, mesh issues, or inconsistencies can affect fabrication. That is why fabrication readiness should not be treated as a final step.
It should be maintained throughout the workflow.
Clean mesh structure
Smooth surface continuity
Stable export geometry
When design and manufacturing align, outcomes improve significantly.
Final thoughts
















Elongation should not be trial and error
Geometry should follow anatomy, not distort it










From Iteration to Intention
Technology should not dilute clinical expertise. It should amplify it.
Traditional socket design is iterative: Adjust→Test→Correct→Repeat. But it does not have to stay that way.
With the right O&P design software, the goal shifts from iteration to intention. Each step becomes clearer. Each decision more controlled.
Not by adding complexity, but by improving Clarity, Consistency and Clinical control.
The future of O&P design software lies in giving clinicians the ability to apply their judgment with greater precision and confidence.
Not through presets.. but through control.
If you are involved in prosthetic or orthotic design and want to explore a more controlled, clinically driven workflow, BenX is currently open for early beta access to a limited group of clinicians.
If this approach aligns with how you think about design, we would be glad to connect.


BenGait Labs Private Limited
Phone
hello@bengaitlabs.com
+91 9971176444
© 2025. All rights reserved.
Products
Legal
Technology
HO D192, LGF, Sector 27, Noida 201301
Regd. Office : B 273, Sector 26, Noida 201301
